Alignment involves identifying common interests and shared goals between an organization’s internal and external components, such as aligning a CE to the healthcare system within which it operates.12 As defined in the Baldrige framework, alignment is “a state of consistency among plans, processes, information, resource decisions, workforce capability and capacity, actions, results, and analyses that support key organization-wide goals.”7
Intentional alignment promotes CE sustainability by interlinking the goals, strategies, systems, culture, needs, leadership, and resources with their surrounding institution. Therefore, the CE’s institution benefits from the CE’s efforts and is motivated to encourage and maintain the CE as an integral part of the overall organization. This approach ensures that all efforts are moving in the same direction and optimizing the CE’s potential to enhance their healthcare system to meet mutually desired outcomes.13,14
Communication
Healthcare organizations and systems are complex, pluralistic environments with competing objectives and diffuse decision-making power. To shape their visions, goals, systems, processes, resources, and tasks and to align motivations, CEs must communicate with leaders within their health system. These include executives, administrators, and healthcare providers. CEs should also communicate with key stakeholders such as patients and families, community members, and policymakers.
Attaining alignment can be challenging. The process of alignment will often require CEs to go beyond the scope of work outlined initially in the grant proposal or organizational charter to deploy solutions and collaborate with their healthcare system. For example, CEs can meet organizational needs that may fall outside the direct research interests of their center, developing practical resources that would be beneficial to other departments, centers, or schools.
Communication between CEs and the governing decision-makers is difficult due to the siloed nature of healthcare systems.13 There are often many degrees of separation between research centers and the governing decision-makers. A 2018 study on implementing patient-centered care through large-scale cultural transformation detailed how alignment and integration of patient-centered care within an organization were major challenges, especially when considering staff roles, priorities, and bureaucratic rules.14 To facilitate long-term continuity, CEs are well positioned to provide the bridges and linkages needed to unify these siloes, thus enabling strategies to overcome known system challenges.
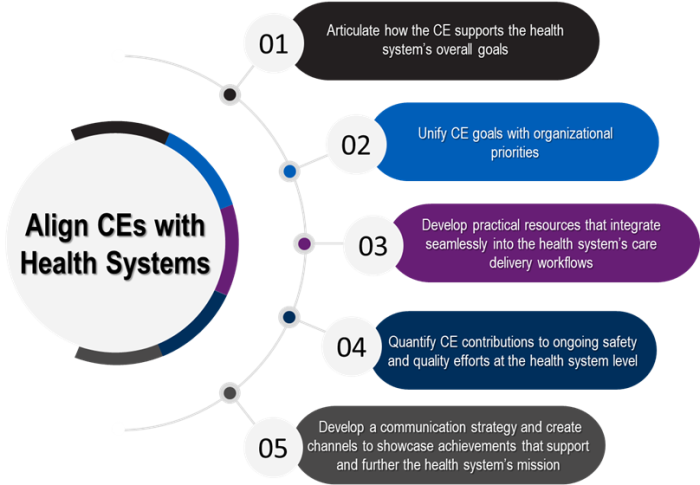
Exhibit 2. Five actions to align CEs with health systems.
Guiding Questions for Alignment
- Are relevant healthcare executives and other leaders aware of the existence of the CE and its activities?
- What strategic priorities and regulatory mandates of healthcare delivery and research enterprises can the CE support?
- Which healthcare organization, research enterprise, or education enterprise leaders does the CE need to establish relationships and communicate with to seek or demonstrate alignment?
- Board of trustees and C-suite members (chief executive officer, chief nursing officer, chief medical officer, chief operating officer, chief financial officer, chief medical informatics officer).
- Medical school dean, department chairs, accountable care organization leaders.
- Patient and family advisory council.
- Directors of residency programs, malpractice insurance captive, risk management, etc.
- Can a CE’s work align with the existing teams within its health system to aid their efforts to improve care delivery, such as quality, safety, or other improvement teams? If so, can the CE clearly delineate a pathway to contribute to mutual goals?
- What additional resources can a CE produce that advance excellence in care delivery and everyday operations of other departments, centers, schools, and its overall health system?
Creating Resources in Alignment With Health System Goals: Johns Hopkins Center for Data Science in Emergency Medicine
The Johns Hopkins Center for Data Science in Emergency Medicine developed a shared data normalization resource in alignment with organizationwide goals. We discussed the program in an interview with Dr. Jeremiah Stephen Hinson, Associate Professor of Emergency Medicine at Johns Hopkins University School of Medicine. He emphasized that aligning goals, strategies, and systems affirmed the Johns Hopkins Center for Data Science in Emergency Medicine as a valuable organizational resource and asset.
The Center for Data Science is a collaboration between the Johns Hopkins School of Medicine and the Malone Center for Engineering in Healthcare. Their shared resource normalized data for research purposes, enabling inter- and intradisciplinary collaboration. Researchers from differing disciplines can use this resource in exchange for contributing data to the shared resource, collaborating with center researchers, and highlighting its use in publications.



