Integration is carrying out alignment by sharing resources (capital, information, and people) and using common workflows to achieve shared goals. Integration occurs across clinical care, administration, research, and community boundaries where coordination and collaboration have not always been realized. According to the Baldridge framework, integration refers to “the harmonization of plans, processes, information, resource decisions, workforce capability and capacity, actions, results, measures, and analyses to support key organization-wide goals.”7 Integration is both a successful end state for a high-performing CE and a strategy for sustainability.
Daily Operations
Actively integrating a CE’s efforts into the daily operations of the health system should improve quality and safety and enhance sustainability for the CE.15 Integrated, multidisciplinary teams facilitate communication and synchronize improvement efforts across existing silos to promote CE and health system goals. An interdisciplinary team of champions, including clinicians, patients and families, and other non-healthcare professionals and executive leaders, is most effective.16
Integration may require creating new models of sharing staff across clinical teams, operations leadership, quality and patient safety, research, and the CE. These may include clinical or operational hires into the CE, support from the CE for portions of health system employee time, or changed reporting relationships within the system. Doing so further embeds the CE into the health system. Integration requires creativity; CEs can brainstorm new ways to promote quality and safety within their healthcare system’s essential workflows and integrate those areas’ leaders into their centers.
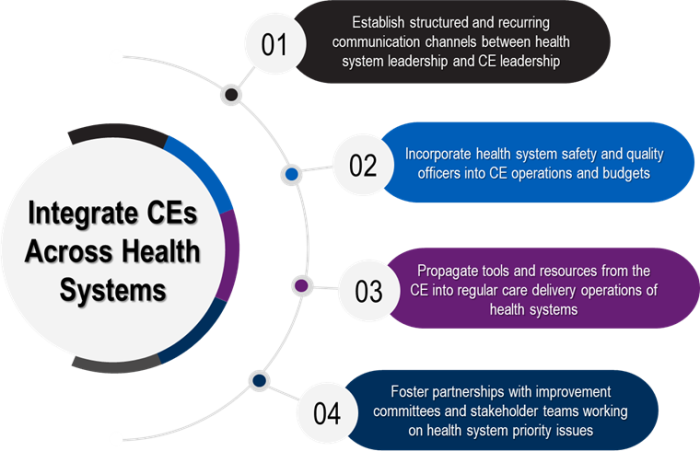
Exhibit 3. Four actions to integrate CEs across health systems.
Guiding Questions for Integration
- What is the preferred model for integration for the CE? Examples include:
- Resource for the healthcare delivery system (e.g., internal experts and consultants).
- Primary research enterprise with minimal integration.
- Primary operationally and clinically focused center with leaders integrated through partial full-time equivalent allocations.
- Primary partner for the quality and safety department.
- What are the priority activities and percentage of work effort allotted to each for the CE?
- Research vs. development of improvement tools.
- Deployment of evidence-based practices.
- Training and education of various stakeholders.
- Ownership of care outcomes, etc.
- How is the CE building capacity for diagnostic excellence within the healthcare delivery organization?
- Interprofessional training and education on diagnostic excellence competencies.
- Undergraduate, graduate, and continuing medical education for diagnostic expertise.
- Clinical decision support, clinical protocol, and other system tool development for diagnostic improvement.
- What collaborative efforts are currently underway, and which others can the CE undertake to partner with system stakeholders to improve quality and safety?
- What processes are in place for shared priority setting and shared workflows?
Integration Leads to Sustainable Success: Pursuing Perfection at Cincinnati Children’s Hospital Medical Center
Getting people to talk to each other, breaking down silos, and getting people to work across units [is frustrating]... Hospitals really do have silos, and they are there for good reasons. What would be ideal is a tunnel that goes all the way across that would allow us to share each other’s goals. You need a dynamism that takes people out of the structure and creates a new way of doing things.
—Manager from a Robert Wood Johnson Foundation Pursuing Perfection Grantee Site17
Cincinnati Children’s Hospital Medical Center (CCHMC) participated in the Robert Wood Johnson Foundation’s (RWJF) Pursuing Perfection (P2) Grant Program, a major initiative created in 2001 in response to the Institute of Medicine’s 2001 Crossing the Quality Chasm report.8,18 The P2 initiative drove change across many healthcare organizations to implement care that was highly reliable, safe, equitable, efficient, and supportive of patients and families.17 P2 participating healthcare organizations achieved dramatic improvements in patient outcomes by making major changes within their system to drive the efficiency and effectiveness of healthcare delivery.17,18
CCHMC was able to make substantive improvements in the quality and efficiency of care through this structured initiative. Maria Britto M.D., M.P.H., Principal Investigator (PI) on the CCHMC P2 Initiative, shared details of their success story.
The P2 grant program required Dr. Britto, as the P2 PI, to report directly to the chief executive officer (CEO) of the health system. This requirement led to collaboration to boost efficiency and quality while the grant was active. This alignment between the goals of the PI and the goals of CCHMC’s CEO led to some program initiatives being funded by the hospital after the P2 grant ended.
Employing an integrated workforce was key to their success. The workforce engaged with the grant and research work was integral to health system delivery and decision making: the chief of staff, division directors, thought leaders, lead clinical working groups, etc. Rather than hiring new people, the CCHMC’s P2 team decided to use grant money to fund a portion of the salaries of physicians and executives who were already integral to care delivery within the health system. This approach was strategic because these individuals have assets that a new hire would not have: organizational knowledge and influence.
This internal recruitment and placement supported the quality improvement work outlined in the grant. The P2 team at CCHMC also coordinated with the CEO’s office to understand how their work to reduce surgical infections could not only benefit patients but also generate revenue for the hospital. Through this partnership, the P2 team found that surgical infections lead to longer recovery times.
While the patient’s recovery is prolonged, they occupy a bed on the surgical floor, which means that higher rates of surgical infections lead to fewer overall surgeries, because infections lengthen patients’ recovery times, reducing the number of available beds for new patients. In addition to the patient harm caused by infections, the P2 team showed that they are a major opportunity cost for the hospital. Thus, the team created a business case for the program: reducing infections helped the hospital increase the surgery unit bed turnover rate, which increased surgery volume.19
Further, alongside the CEO’s office, they found that some of the initiatives they developed improved the quality and efficiency of care but were not revenue generating for the hospital, such as preventing nonessential surgeries. The transparency of communication on whether an initiative was revenue generating built trust between the P2 team and CCHMC’s CEO. The CEO told the P2 team to prioritize making patients healthier and let the business team work on paying for it.18
The CCHMC example of integration shows how building a team of people who are integrated throughout the healthcare system can lead to sustainable programs beyond the duration of initial funding. Here, the vast improvements in quality became the standard of practice for the healthcare system because of careful efforts to align the goals of the P2 grantees and stakeholders within the health system while integrating those stakeholders into the operations of the P2 grant.
“PIs and delivery leaders need to be in consistent communication so that they are aligning to the granularities of the challenges their health systems are facing.”
—Maria Britto MD, MPH, Cincinnati Children’s Hospital Medical Center



